Finally, a straightforward guide to help you buy antibiotic-free meat. If you’re not raising your own livestock, here’s how you can be sure there are no antibiotics in your meat…
Today, the steak on your plate was raised from a baby calf to butchering weight at speeds that would astound your ancestors.
“Bigger, faster, cheaper” is the mantra of the commercial meat industry, and one key to their success has been the widespread use of antibiotics.
Livestock fed a steady diet of growth-promoting antibiotics can put on weight at impressive rates, but recently scientists are sounding the alarm about the consequences of feeding these powerful medications to essentially healthy animals.
Concerned with the rising risk of antibiotic resistance, many scientists believe that feeding significant doses of antibiotics to livestock has dire rammifications for both human health and modern medicine.
The risk of creating superbugs (microbes so powerful that known antibiotics can’t keep them in check) is too real to ignore, and warnings are coming out that unless we begin to take antibiotic resistance more seriously, modern medicine may lose its effectiveness in the next hundred years.[i]
The stakes are high, so take the time to educate yourself about the use of antibiotics for livestock to learn what’s really happening to the animals that become your dinner.
The Mixed Blessing of Antibiotics

Antibiotics are medicines that destroy bacteria, making them useful for controlling, treating and even preventing disease and infections.
In the decades since their discovery, antibiotics have saved millions of lives because simple cuts are no longer a death threat, and invasive surgeries and once unthinkable organ transplants are now routine.
Unfortunately, almost eighty years of global antibiotic use is starting to reveal some downsides.
Because antibiotics work by killing off entire populations of bacteria within your body, they essentially destroy all bacteria within range. However, bacteria are living organisms that have random genetic variances that equip a few out of millions to survive the onslaught of specific antibiotics. These surviving bacteria then become the ones that propagate, and consequently spread their resistant genes.
Over time, entire populations of bacteria become resistant to multiple forms of antibiotics, which makes them SUPERBUGS.
Because they are resistant to most common antibiotics, superbugs are incredibly difficult to control. They are responsible for an estimated 700,000 deaths annually, and that number is expected to rise to over 10 million by 2050.
For this reason, the World Health Organization recently listed antibiotic resistance as a major global threat for the 21st century.[ii]
Out Of Control: Superbugs and the Meat Industry

[UPDATE, December 15, 2017: The U.S. Food and Drug Administration’s Veterinary Feed Directive Final Rule went into effect on January 1, 2017. The rule aims to reduce antibiotic resistance by eliminating the common practice of using “medically important” antibiotics to promote animal growth and feed efficiency. However, with the approval of a veterinarian, livestock producers may still feed these antibiotics in therapeutic dosages to prevent the illnesses fostered by the less-than-desirable living conditions often found in commercial operations. For more information on this topic, I strongly encourage you to read Angie’s well-balanced comment below. She offers an excellent perspective!]
The root of the problem of antibiotic resistance comes from an overuse of antibiotics themselves, and one of the ways that antibiotics tends to be overused is with livestock.[iii]
While humans need a prescription to gain access to antibiotics, farmers aren’t under the same requirements for their animals and can administer them with minimal regulation. (Please see the update at the beginning of this section.) In 2011, almost 30 million pounds of antibiotics were used for animal production, which was almost four times the amount used by the national human population.[iv]
Why are so many antibiotics given to animals?
In past decades livestock producers began to use them as a preventative measure to keep their animals healthy against infectious disease, something that became increasingly important as factory farms kept animals in tight living conditions.
They later found that small daily doses of certain antibiotics made animals grow bigger and faster, often gaining as much as 3 percent more weight than otherwise possible.[v]
Consumers may like cheap meat, but feeding excessive amounts of antibiotics to animals has some dire consequences for human health.
The growing threat of antibiotic resistant strains of bacteria from the overuse of these drugs can compromise the effectiveness of treatments for humans, putting the reliability of life-saving drugs at risk for the people that need them most.
China and Colistin: An Example of Bacteria Gone Bad

To understand the true threat of antibiotic resistance, you only need to travel over to China to get a glimpse of what the damage can be.
Recent reports have shown that Chinese strains of E. coli (a diverse, often dangerous strain of bacteria) is showing resistance to an old form of antibiotic called colistin.[vi] Discovered in the 1950s, colistin fell out of favor when antibiotics with fewer side effects were discovered. However, as preferable medications continued to be compromised by antibiotic resistance, colistin use became widespread again. Unfortunately, even this trusted antibiotic is becoming vulnerable to E. coli superbugs.
The growing problem with colistin resistance is traced back to the Chinese meat industry, where over 8000 tons of it are given to pigs and chickens every year to enhance their growth.
Strains of resistant E. coli have been found in meat, livestock and even people around the world, and the threat is real that the colistin resistant gene in E. coli could spread to other dangerous bacteria as well. The danger doesn’t just stay near farms, either.
Manure tainted with drug-resistant bacteria often infects nearby water systems.
And flies often carry the bacteria to cities far away, sometimes even to already vulnerable hospital patients.[vii]
Sick From Tainted Meat:
Modern medicine losing its potency has dire consequences for everyone on the planet, and the effects for your health should be a top concern.
Widespread antibiotic resistance in livestock means that dangerous pathogens aren’t always killed off before meat makes it to your plate. A 2001 report from the New England Journal of Medicine found that 20 percent of ground meat in supermarkets contained salmonella, and 84 percent of that salmonella was resistant to one or more antibiotics.
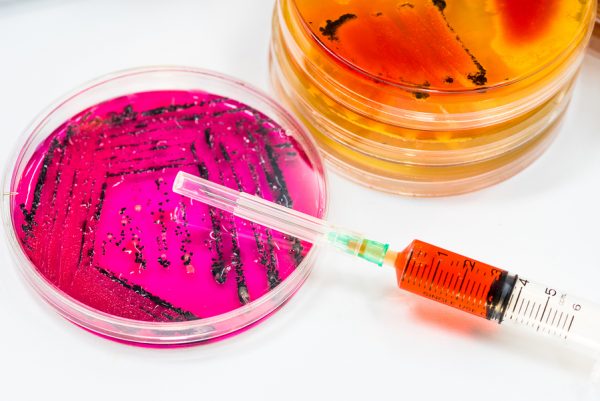
A 2001 report from the New England Journal of Medicine found that 20 percent of ground meat in supermarkets contained salmonella, and 84 percent of that salmonella was resistant to one or more antibiotics.[viii] The situation is similar for poultry. Consumer Reports tests of chicken from 2006 and 2012 revealed that over two-thirds of their samples were contaminated with salmonella, 60 percent of which was resistant to forms of antibiotics.[ix]
Though the meat industry believes these statistics aren’t concerning, because people thoroughly cook their meat before eating it, partially raw meat, unwashed cutting boards, or thawing meat juice that leaks onto other foods in the refrigerator are all ways that pathogens can spread.[x]
More Drug-Resistant Diseases
Humans and animals swap diseases all the time. A full two-thirds of human diseases first began in animals, and drug resistance that starts with animals can also jump the species boundary.[xi]
Evidence is now growing that resistant bacteria from antibiotic treated farm animals can spread to the humans that eat them. This means that ingesting drug-resistant bacteria in meat that wasn’t fully cooked might make you ill with a disease that antibiotics are powerless to treat.[xii]
The problem is only growing. The Centers for Disease Control and Prevention have found that over two million Americans become sick with drug-resistant bacteria every year, and more than 23,000 end up dying.[xiii]
The connection between the increased use of antibiotics for meat production and the loss of effectiveness of human medicine is becoming better understood, and the evidence is clear that feeding unregulated amounts of antibiotics to livestock is only going to harm human health in the long run.
The threat of looming antibiotic resistance is real, but those in authority aren’t always acting in the public interest. According to the Natural Resources Defense Council,[xiv] the FDA has buried research findings that revealed 18 types of antibiotics currently used on livestock that carry a high risk of increasing the levels of antibiotic-resistant bacteria for diseases that affect humans.
Even worse, many of these medications don’t reach the FDA’s own safety standards, yet they are used widely on livestock across the country.
Best Ways to Source Antibiotic-Free Meat:
In recent years, consumer outrage against antibiotics has created positive changes in the food industry.
Three of the largest chicken producers in America (Tyson, Perdue and Foster Farms) recently stated that they intend to reduce the amount of antibiotics fed to their healthy birds.
Large corporations like McDonald’s,[xv] Wendy’s and Popeyes are also taking a stand against fluoroquinolones (a family of synthetic antibiotics) and are refusing to buy birds that have been treated with them.[xvi]
However, there’s still no way to know for sure if these brands are sticking to their promises and keeping antibiotics out of their products.

If you want to reject antibiotics in your meat, you’ll need reliable ways to source antibiotic-free alternatives.
(Assuming you’re not ready to start raising your own livestock, which is what we ultimately recommend)
If you are ready to consider raising your own meat, check out or video”How To Produce ½ Of The Protein for a Family of 4 In Less Than 10 Minutes per Day”
Reading The Labels:

To ensure that the meat you eat doesn’t contain trace amounts of dangerous bacteria, you need to familiarize yourself with the following methods of identification.
- Country of Origin: Depending on where your meat is sourced from, it might automatically be safe from antibiotics. Since 2006, European Union has banned farmers from using antibiotics to promote growth and instead regulates their use to treating disease only.[xvii]
- USDA Organic: When organically-raised animals become sick, they are treated with antibiotics and sent to a conventional production system where they are no longer labeled as organic. This means that any meat product with the label USDA Organic is guaranteed to be free of antibiotics, both for promoting growth and for treating illness.[xviii]
- ‘Raised Without Antibiotics’, ‘No Antibiotics Administered’ and Similar Variations: These labels signify that the meat in question came from animals raised without antibiotics, often in conditions comparable to organic (but uncertified). For extra reliability, look for labels accompanied by a “USDA Process Verified” shield, which ensures that the company in question paid to have their claims verified.
Labels to Avoid When Buying Antibiotic-Free Meat
There’s lots of money to be made selling shady meat, which is why healthy sounding labels that are actually meaningless abound in the supermarket. If you really want to source meat that’s free from antibiotics, be sure to avoid these convincing, yet empty, claims.
- Antibiotic-Free: The USDA has never legally authorized the use of the term “antibiotic-free”, so if you see it on packaging it has no legal meaning.
- Natural: The USDA meaning of natural is very loose, and only implies that the final product is minimally processed and doesn’t contain added colors or artificial ingredients. Antibiotics are fully allowed in “natural” meat, making the term meaningless if you’re trying to avoid them.
- No Antibiotic Residues: Though this isn’t a USDA-approved claim, it’s often used on labels to refer to the fact that antibiotics were not used for the last days or weeks of the animal’s life so that traces of the chemicals would have time to naturally work themselves out. However, the label “No Antibiotic Residues” usually implies that the animal was fed significant amounts of antibiotics earlier in life.
- No Antibiotic Growth Promotants: Not only is this claim not approved by the USDA, it’s also intentionally misleading. Animals that aren’t given antibiotics to aid their growth levels might still get them regularly to stay healthy in their crowded cages, meaning their exposure levels are far higher than the label implies.[xix]
The growing threat of antibiotic resistance is likely to only get worse.
To cut out the biggest source of antibiotic use and keep the planet safe, do what you can to buy antibiotic-free meat. Better yet, raise your own livestock.
It’s not an exaggeration to say that the continuation of modern medicine might someday depend on it.
(This article was originally published on March 31, 2017.)
Sources
[i] The Biggest Threat to Modern Medicine- Antibiotic Resistance
[ii] World Health Organization: What to Do About Resistant Bacteria in the Food Chain
[iii] STAT- The Livestock Industry is Key in the Race to Fight Antibiotic Resistance
[iv] Consumers Union: The Overuse of Antibiotics in Food Animals Threatens Public Health
[vi] Flies are Spreading Antibiotic Resistance From Farms to People
[vii] Flies are Spreading Antibiotic Resistance From Farms to People
[viii] The Isolation of Antibiotic-Resistant Salmonella from Retail Ground Meats
[ix] Consumer Reports: The High Cost of Cheap Chicken
[x] Superbug Resistant to Last Resort Antibiotic Arises in China
[xi] 13 Animal-to-Human Diseases Kill 2.2 Million People Each Year
[xiii] Center for Disease Control: Antibiotic/Antimicrobial Resistance
[xiv] NRDC Petitions FDA: Agency’s Weak Attempt to Curb Antibiotic Abuse in the Livestock Industry is Failing
[xv] McDonald’s Now Serving Chicken Raised Without Antibiotics-Mostly
[xvii] European Commission: Ban on Antibiotics as Growth Promoters in Animal Feed Enters into Effect
[xix] Consumer Reports: Antibiotics in the Meat Industry
In 2008, Alayne left the city for the rural life. She is thankful to have some acreage to spread out, live more sustainably, and start a garden. Alayne is a freelance writer, who lives outside of Lockhart, Texas and enjoys writing about locally grown food, cooking, nutrition, natural health, and the environment. Homeless dogs have a spot in Alayne’s heart, as she has rescued more than she cares to mention. She is making up for lost time, since she didn’t get started with vegetable growing until recently. Now, she is all in with greenhouses, raised beds, starting vegetable seeds, growing herbs and trees, and learning about the wild edibles growing around her. You can visit her at www.kitchenchat.net.









COMMENTS(17)
Frightening!
Hi Marjory,
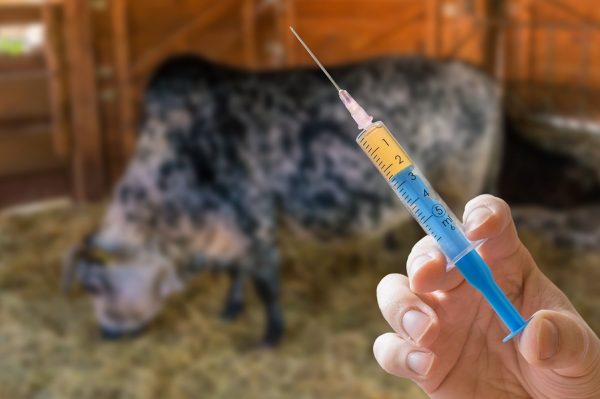
As always you have written a very informative article, but there were a couple spots that I did question the wording. One spot was at [iii] “…one of the ways antibiotics are used carelessly is with livestock.” Most producers aren’t careless. They are taught to believe that antibiotics are the best way to get their livestock to market faster. Another place was at [vii] “And flies often carry the bacteria to cities far away…” The article referenced said that sick people were showing up in the cities with resistance and that “in the summer flies will carry those bacteria everywhere.” I also question the source of one of your pictures, the one with the needle in the foreground and a bovine in the background. That is NOT the type of needle used to treat large animals. I raise cattle and a needle that small and thin is useless, plus most antibiotics are added to premixed feeds not injected. Injections are used for sick animals only on our farm and then they are never shipped from our place before the withdrawal period is over. We also don’t feed premixed feed, we grow our own.
Just some thoughts.
Marjorie, you don’t mention “grass-fed” beef. I buy from a local farmer who publishes that label. Is it meaningless, too? I need to ask him about the antibiotics issue, but thought I was doing right buying from him. Also Publix offers beef tagged “Greenwise.” I thought that meant antibiotic-free. Should I address that question to Publix?
Kitty Corbett,
The grass fed label isn’t meaningless, but it refers to whether the animal was fed grass vs. grain, not whether it was given antibiotics or not. Pasture raised animals often aren’t given antibiotics, but you’ll have to ask your farmer to be sure. And regarding Publix, as far as I know, their “Greenwise” beef is just their store brand label. I don’t think it has any meaning beyond that. You’ll definitely have to ask the store. Hopefully I was able to help answer your questions.
Great report. As a person with multiple allergies and especially to drugs and synthetic substances, back in the 1980’s I joined a Sufi community and we grew our own cow for milking and calves for beef and also sheep. I learned just how good that meat tasted and how much healthier I began feeing. I also learned about homeopathy from a visiting speaker and began to use that and that is how I deal with illness. I married there and later moved to Los Angeles and began to get sick and learned what was being put in the animals and with difficulty switched to organic meat and fresh local fish and produce from local small stores where you could ask about their practices. My health improved and then got worse when we moved to the south until I found a nearby health food store where those of us concerned with the quality and safety of our food encouraged the expansion of options for healthy meat and produce. Now our town is a leader for encouraging home gardening and community gardens and the options for healthy eating is expanding with educational talks at the weekly market by the library helping people realize it is not out of their budget to eat healthy. The dangers now are eating out and exposure to disease from that at group events or when traveling. Today it is essential to ask questions at local restaurants and to travel defensively by carrying safe items with you and researching where to make your stops so that you can go to a health food store or market. As you do this and speak openly about it to family at holidays and to friends at pot-lucks you can help others to learn how to eat safely and they in turn tell others and it leads to the support of the organizations who are making it their job to keep us informed about what is new as well as how to let elected officials know that your vote will change if they do not support measures to protect our water and food supply. Thank you for the wonderful work you are doing.
Hi Mary, Where do you live. I’m looking to relocate and it sounds like a wonderful place.
Hi Majory!
Just a few things I feel need to be addressed about this post.
The majority of antibiotics used in livestock DO require a veterinarian prescription. There are only a handful of antibiotics, like penicillin and oxytetracyline, that do not require the vet to sell them to a farmer. Regarding these OTC antibiotics, such as penicillin, many governments are now enforcing regulations on the farmer for their purchase. For instance, the producer needs a number in many areas (PID, VFID, etc.), which they are required to register for, to purchase any OTC antibiotics. Even things like Blue Kote spray or medicated calf milk replacer, for instance.
The prophylactic use of abx within industrialized farming is out of control, but to distinguish between “growth promoting” and prophylactic drugs is hard to do. The reason “growth promoting” antibiotics are so helpful with growth is simply because they are keeping that animal healthy. They are lowering incidences of liver abscesses in cattle fed high grain diets for instance, which make the animals healthier and thereby, they grow better. The only distinction you seem to be giving between growth promoting abx and prophylactic abx is the insinuation that the ones fed in the animals feed are growth promoting while the ones injected are not (although you don’t say this explicitly). However, whether the animal gets that abx vie eating or injection, an abx is and abx and they are all doing the same thing.
Also, antibiotics used within livestock are on the lowest ranking of importance to people. Common ones are called Ionophores which are considered to have absolutely no medical relevance to human medicine (Although I do realize that could easily change after 20 years of use and proceeding studies)
The biggest thing I find about this blog post though, is how it’s sensationalized.
“A 2001 report from the New England Journal of Medicine found that 20 percent of ground meat in supermarkets contained salmonella, and 84 percent of that salmonella was resistant to one or more antibiotics.”
Besides the mention in the part about e. coli, you fail to mention that Salmonella is a bacteria that is regularly found within human excretion and that for it to get onto ground meat, it could have easily been placed there by HUMAN HANDS. This is why those wash your hands things are everywhere. However those antiseptic dispensers everywhere have been studied to show that they are leading to big resistance for bacterias like E. coli, Salmonella, etc. that are regularly found on human hands. What do you not hear about so much infecting people? Campylobacter and Cryptosporidium are two options that are very common in many cattle, almost more so than e. coli or salmonella, why aren’t people being infected with those if the antibiotic use in livestock is a leading cause?
I do believe that animal management practices need to start to change so our reliance on antibiotics to keep the animals healthy is lessened. However I don’t feel that should be done in a manner that makes producers look like they are supplying antibiotics in shady ways, trying to cover it up with unregulated terms, all so they can raise a cheaper meat.
Do we know about Trader Joe’s? I know there have been claims that they do not use antibiotics in any of their meat products. Is this really true?
If you can’t raise your own, seek a farmer that does it right.
The farm I visit, every 2 weeks, has all livestock, chicken, lamb, beef and pork raised on pasture. I get to witness this. Thru cow share I also get my raw milk there. I also have my own eggs from organic feed spoiled chickens and enough garden produce to last from one season to the next. I just never understood the people that balk at paying a little more for clean food but willing to shell out thousands a year on medical issues. Just eat clean food and those bills will go away.
Amen! Why any critically thinking human would choose to eat meat contaminated w/ anything… vs clean, healthy, grass-fed is astounding. Eat cows that eat grass.. not stand in wretched pens being stuffed full of antibiotics, growth hormones, chemical wormers, & pesticides because they’re forced to eat poisoned grains or starve to death. Drive by a feedlot.. or better yet get a tour & get educated. ~signed Clean Beef & Dairy Producer.. who’s family is healthy.
I don’t ever trust USDA anything because the head guy that ovomit placed in there is none other than the head guy that runs Monsanto!!!!!!!! And all your meat from China is very questionable because they DO NOT have any inspections or anyone watching how they process anything over there!! China bought up John Morrell, Smithfield, Cooks, Morning Star, Farmland, and Armour meats!!
The FDA are allowing the food Co.s from letting us know what country they products are coming from!!! So ones should look up NOW where the brand names for your food are!! I did it a few years ago, and who owns them! Everything should say VERIFIED on the labels, and if they don’t be very careful as to what your buying! I’ll bet one day that will not be good enough either if these top 10 Co.s get their hands on them!!! That’s what has happen to a lot of the organic farms. There is a list out there to get of the top 10 bad brands, and the good organic brands to use! Just have to research it! I take a list of ALL the good, and bad products with me every time I go shopping after a while you remember them!!
Pat, it would be REALLY helpful if you included the name/site of the list you mention so we could all check it out. Even some lists i have seen are not 100% correct.
Hello Marjorie,
interesting work, but I think there is something missing. and I have a question for you:
The smallest dose of antibiotic of the quinolone family (the one given to livestock) will make me sick and trigger all the side effects of the drug (see quinolone in Wikipédia). Therefore I am very cautious when I eat meat (and fish).I found out the hard way that, despite the european laws, european meat still contains antibiotic. How come? Aparently, animals are given a shot at birth, and then, there are sold to the farmer who will grow them. The farmer will not give antibiotic to the animals because with the shot they had at birth, they are protected long enough for their short life span (a few months). The drug take months to be fully eliminated by the body.
Therefore, I am wondering if the meat labelled ‘USDA organic’ is really safe: does it mean the animal has never ever received any treatment, even at birth? Or does it mean it didn’t get treatment during its growth phase?
As always she is informing us. Its up to the individual to do their own reaearch if it concerns you. Take charge & be responsible for your health, and know that you do have options. Research everything these days! We certainly cant leave it up to others. So much corruption is going on its sickening! I say this because I WAS naive & uninformed. Unfortunately I learned the hard way, from personal experience! Be Intentional when it comes to your health!!! ☺
Woh! and I just bought two big Cooks bone in Hams on sale at Food Basic. Does anyone know WHERE the best Turkeys, Hams and Meat can be bought.? We had a farm in Ireland 50 years ago before coming to Canada and our chickens, pigs were all fed the grain from our fields. The butter, eggs and of course Potatoes were delicious. Now I find the eggs from the Grocery Store are stale or maybe they are affected by the food given them.
My neighbours would not be happy if I started having chickens, and a cow, maybe a pet pig in our back garden.
Would like to have a good speaker on this topic for our Horticulture meeting.
We have a small family farm… meaning the kids got into 4H showing calves and it stuck. We have a milk Guernsey and breed her and take the calf to raise for food. We can also get a dairy bull calf locally since dairy’s don’t keep them (about $100) and raise them up for meat. We just free range them on our pasture although it does take a dairy calf longer to grass feed and grow to a size enough to butcher but that is fine. We know what is in it. So, it doesn’t take a lot of land if you can find a local dairy to buy a calf. We,also, have dairy goats and sheep, we raise the bucklings and ram lambs for meat or sell. We have just enough to give us an assortment of meat. You would be surprised on what you can do on limited amounts of land if planned out. We tend to learn by lots of trial and error as we decide to add or do something new?
Because I am allergic to so many things and most are to medications such as Sulfites, Sulfates and Sulfonamides and other antibiotics I have to buy Kosher and Organic meats. I have found that I can safely buy Kosher or Organic meats at the Sprouts Market. I have to go almost 400 miles round trip to shop there but there is not other option. Since I use VA and it is near Sprouts we go there when we have Dr. appointments at VA. I buy enough of what we need to buy until the next appointment and freeze it.
If you go the kosher route you will need to buy from a store run by a Jewish community. They are really strict in their kosher laws and will not allow antibiotics or other drugs used in the meat that they butcher. I get the Kosher meat from a small market that is actually in a building of a Synagogue. Their meat is fantastic.
One of the most misdiagnosed allergy is to sulfates, sulfites and sulfonamides. They mimic other problems like chronic pain, arthritis and other problems so Doctors treat for something you don’t have. Believe me I have been through it. I was diagnosed with Chronic pain in 2001. When I started to control what I eat and read the ingredient’s in all I buy not just food and cut out anything with sulfate, sufite’s and sulfonamides (and believe me it is in everything food, soap, shampoo cleaning products etc.) I have been able to cut out the pills I was given for the pain.