The threat of antibiotic-resistant superbugs has become a global concern. Last year, to help countries prioritize their efforts to research and develop new antibiotics, the World Health Organization[i] has created a list of the top twelve most dangerous superbugs.
A panel of international experts[ii] at the WHO used four criteria to determine which disease-causing bacteria made the list:[iii]
- Prevalence in the general community
- Overall mortality rates
- Burden on the health care system
- Level of resistance to treatment
The twelve bacteria that ranked highest on their list are the most dangerous bacteria on the planet today.
The Threat of Antibiotic Resistance
Concern over antibiotic-resistant superbugs[iv] is becoming more and more important. Every year, antibiotic resistance in the United States is responsible for 2 million illnesses and almost 23,000 deaths.[v] Most fatalities come from people with weak immune systems, including cancer patients, infants, and the elderly. A widespread, antibiotic-resistant superbug epidemic is just a matter of time. There are diseases now resistant to every antibiotic we have available.
One reason why the supply of antibiotics has dwindled to dangerously low levels is because new drugs are difficult to create. Seventy years of antibiotic research discovered dozens of effective drugs. But new ones aren’t being developed fast enough to beat the resistant stains. There have been decades of overuse of antibiotics by both humans and livestock. It’s easy to see that a perfect storm of antibiotic-resistant superbugs is brewing.
New Antibiotics?
Pharmaceutical companies aren’t likely to create new antibiotics anytime soon. They take years to develop[vi], and most aren’t profitable enough for drug companies to invest millions in research and development. There has not been a new antibiotic brought to the market since 1984. It looks like there is less of a chance that a new “miracle drug” will be on the market anytime soon.
Nonetheless, the stakes have never been higher to become better prepared to fight against antibiotic-resistant superbugs.
The superbugs that made the WHO list are separated into three categories: critical, high, and medium.
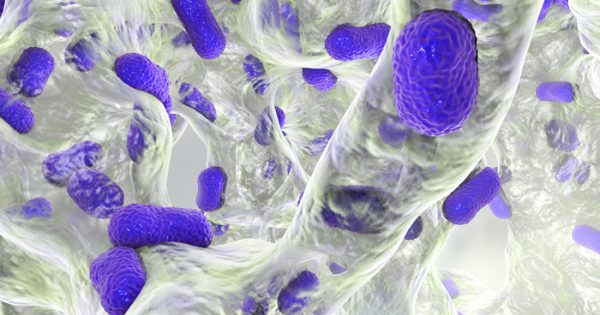
Acinetobacter baumannii © Kateryna Kon
Priority 1: Critical
According to the WHO, there are three types of superbugs that require immediate attention in order to keep them under control. They are categorized as a critical priority because each one is multi-drug resistant and often prove fatal in hospitals and nursing homes.
1 Acinetobacter baumannii, carbapenem-resistant
Acinetobacter baumannii is highly drug resistant and affects people with compromised immune systems, meaning it often leads to pneumonia and is increasingly responsible for deadly blood infections in hospital patients.
2 Pseudomonas aeruginosa, carbapenem-resistant
Highly adaptable in developing antibiotic resistance, pseudomonas aeruginosa is responsible for skin rashes, ear infections, blood infections, and often deadly bouts of pneumonia in hospital patients.
3 Enterobacteriaceae, carbapenem-resistant, 3rd generation cephalosporin-resistant
As a family of bacteria often found in the human gut, enterobacteriaceae has been called a “nightmare bacteria”[vii] by health officials. It is resistant to over a dozen antibiotics and kills half of all infected patients. Hospitals are the main place to contract enterobacteriaceae. It is known to cause urinary tract infections and pneumonia.

©Eldar Nurkovic
Priority 2: High
Next on the WHO list are a variety of multi-drug resistant microbes that spread quickly and are dangerous to contract, including staph infections, salmonella, and gonorrhea.
4 Enterococcus faecium, vancomycin-resistant
Though often harmless in the human intestine, enterococcus faecium can also cause dangerous diseases like meningitis and endocarditis.
5 Staphylococcus aureus, methicillin-resistant, vancomycin intermediate and resistant
More commonly known as MRSA[viii], staphylococcus aureus is the bacteria responsible for roughly one third of flesh-eating bacteria[ix] in the United States. This superbug is a prime cause of skin and respiratory infections and food poisoning. Often it is resistant to penicillin. MRSA is regularly found[x] in hospitals.
6 Helicobacter pylori, clarithrocin-resistant
Often present in the stomachs of people with gastric ulcers, helicobacter pylori has been linked to stomach cancer.[xi] The majority of infected patients don’t show any symptoms. Strains of antibiotic-resistant helicobacter pylori are becoming more common, making effective treatment very difficult.
7 Campylobacter, fluoroquinolone-resistant
Found in poultry, campylobacter[xii] spreads to people who eat the contaminated meat. This microbe causes blood diseases, diarrhea, and food poisoning, especially in developing countries that do not have access to proper antibiotics.[xiii]
8 Salmonella spp., fluoroquinolone-resistant
Found worldwide, strains of salmonella cause a variety of illnesses, including typhoid fever and food poisoning. Throughout the U.S., an estimated 1.4 million people[xiv] become ill from salmonella every year. Infants, young children, and the elderly are most at risk.
9 Neisseria gonorrhoeae, 3rd generation cephalosporin-resistant, fluoroquinolone-resistant
Shaped like a coffee bean, neisseria gonorrhoeae is responsible for an antibiotic-resistant superbug of the sexually transmitted disease gonorrhea. Antibiotic resistance against penicillin was widespread by the 1940s. Today most forms of neisseria gonorrhoeae are resistant to every drug but cephalosporin, which is “the last line of defense.”[xv]

©VadimGuzhva
Priority 3: Medium
Childhood infections make up the “medium priority” for the WHO. However, many researchers fear that antibiotic-resistant superbugs will soon become more widespread.
10 Streptococcus pneumoniae, penicillin-non-susceptible
While Streptococcus pneumoniae is relatively common in the lungs of healthy people. However, those with weaker immune systems (like children and the elderly) often come down with pneumonia, infections, and meningitis.[xvi]
11 Haemophilus influenzae, ampicillin-resistant
Once thought to be the cause of the flu, haemophilus influenza is still known as “bacterial influenza.” Actually, it’s responsible for infections like bacterial meningitis, pneumonia, and infectious arthritis. It is resistant to penicillin antibiotics.
12 Shigella spp., fluoroquinolone-resistant
Naturally found in humans and gorillas, shigella is a leading cause of diarrhea worldwide. It contributes to 74,000 to 600,000 deaths every year.[xvii] Many of the antibiotics used aren’t working any longer.
The looming threat of antibiotic-resistant superbugs is a medical issue likely to be the talk of the 21st century. The WHO hopes that making this information public will help bring proper research and new discoveries in the fight against these antibiotic-resistant superbugs.
(This is an updated version of an article that was originally published August 3, 2017.)
[ii]The Washington Post: The World’s Leaders are Finally Holding a Summit on Superbugs
[iii]Stat News: WHO Releases List of World’s Most Dangerous Superbugs
[iv]New York Times: Deadly, Drug-Resistant “Superbugs” Pose Huge Threat, W.H.O Says
[v]Center for Disease Control and Prevention: Antibiotic Resistance
[vi]IDSA: Despite Superbug Crisis, Progress in Antibiotic Development ‘Alarmingly Elusive’
[vii]PBS Frontline: Illinois “Nightmare Bacteria” Outbreak Raises Alarms
[viii]New York Times: MRSA Health Guide
[ix]New York Times: Necrotizing Soft Tissue Infection Health Guide
[xi]Pathobiology of Helicobacter pylori-induced Gastric Cancer
[xii]Medscape: Campylobacter Infections
[xiv]Human Health Implications of Salmonella-Contaminated Natural Pet Treats and Raw Pet Food
[xv]Planned Parenthood: STD Awareness: Antibiotic-Resistant Gonorrhea
[xvi]New England Journal of Medicine: Community-Acquired Bacterial Meningitis in Adults
[xvii] Status of vaccine research and development for Shigella
More Antibiotics are Not the Answer!
Do you know how to treat common injuries and infections without the help of a doctor or antibiotics?
Unleash Infection-Fighting Compounds
Hundreds of Millions Of Years In The Making!
Click here for more information

The Grow Network is a global network of people who produce their own food and medicine. We’re the coolest bunch of backyard researchers on Earth! We’re constantly sharing, discovering, and working together to test new paths for sustainable living—while reconnecting with the “old ways” that are slipping away in our modern world. We value soil, water, sunlight, simplicity, sustainability, usefulness, and freedom. We strive to produce, prepare, and preserve our own food and medicine, and we hope you do, too!









COMMENTS(15)
Antibiotics are passed out like candy these days… great information.
As hard as we try- and we must keep trying we are in the last days of this earths history. Health issues are out of control. The best – only thing we can do is rely on God’s power to see us through. He gave us knowledge about herbs wherein lies our only safety. Diet is our only other option.
In the book The Great Controversy by Ellen G. White she states what man is finding out now nearly 100 years later that “we will grow what we eat and eat what we grow”. Times will get so bad just before Jesus comes He will have to feed us. The Bible states -KJV- “our bread and water will be sure “. We will know hunger weariness and delay so we must grow our faith now and get a focus on survival and where we are headed. Soon the storm will break relentless in its fury and who will be able to stand. Memorize Psalms 91.God Bless your efforts.
Thanks for providing this valuable information. On a slightly different but related note, I encourage your readers to learn about Clostridia bacteria; particularly Clostridium difficile (C-Diff), a serious infection, which is quite prevalent and can be challenging to treat.
My husband and I provided a home for a man. He requested the room closest to the bathroom. I work in health care and have experience with C-diff. C-diff has a distinctive smell. I could smell C-diff. He told me he had this problem ever since he had been in the hospital. I gave him colloidal silver (500ppm) 1/4 teaspoon 4 times a day. C-diff was gone within a week. C-diff drains you on electrolytes and nutrition…..can be deadly.
You should really look into Silver Colloid. It is effective against most of all these horrendous illnesses.
I got MRSA from a shopping cart. By the time I got home with my groceries four of my fingers were rotting. I treated both hands right away with Eucalyptus essential oil. My hands were completely healed within three days.
MRSA can be community acquired. It can be in playground dirt and mulch. Dogs can carry it in their noses so don’t let them lick or snuffle on you with an open wound. The visiting “therapy dogs” going from bed to bed in nursing homes and hospitals always made me want to scream. Retired now and don’t have to worry about that.
thank you, not just for the info but the timelyness. I’ve been informed of a cousin who is currently dealing with MRSA. Not sure just what I can do at this point, except that I’m going to teach his wife how to make bone broth to build up his immune system.
Thanks again,
Dee
Hi there~
Just helped my hubby overcome a MRSA infection on his skin that was forming fast. 1 tsp tumeric powder in 1/2 glass warm water 3x daily, 1 diced clove garlic (raw is a must) in a bit of honey 3x daily (or more depending on severity of infection), topically i applied garlic salve, tea tree oil, charcoal compresses and tumeric paste (tumeric with cayenne, garlic powder, oil). Continue until 2 days after infection has cleared. Hope this helps a little at least! Oh, also echinacea tea, 1 tbsp herb per 6oz water, to help build up immune system, and 3x 1000mg of vitamin c a day.
* I am a Holistic Health Practitioner/Herbalist/Nutritionist* Incase that matters to ya! 🙂
What’s Going down i am new to this, I stumbled upon this
I’ve discovered It positively helpful and it has aided me out loads.
I am hoping to contribute & aid other customers like its aided me.
Great job.
My brother suggested I would possibly like this web site.
He was once entirely right. This put up actually made my day.
You cann’t believe simply how a lot time I had spent
for this information! Thank you!
It scares me that every time I walk into a hospital, i.e. Cleveland Clinic, I have some type of new cold or flu or whatever.A lot of superbugs can be caught in the hospital. You come to the hospital to get healthy and you will walk out with a lethal disease without a cure. Big Pharma and Medicine will never provide the answers. Only we, the people, following nature and proven natural remedies will consistently be able to get our bodies well and not produce some new and greater horror like a Superbug.
Do the 2 DVDs help us know how to treat the above mentioned super bugs?
I would just like to share this with people who understand and appreciate it. In April 2015 I suffered a mini stroke from too much salt intake as a remedy for cramps. Bananas, potassium and whatever else proved ineffective or too expensive. Courses of High blood pressure medications followed and in November ’15 I went for an elective hip replacement.
I spoke to a doctor about the cramps, thinking he may help with something. He literally gave me a dirty look and turned on his heel. I kid you not. From the next day I received a cup of jelly and a fruit. Long story short, on my own conclusions, I am now on 4 teaspoons of gelatin per day since then – not desert jelly, it has 96% sugar content. Half a mug of hot water, mix, then cold water to fill, toss it, slight glue smell and be done.
The result is that the cramps disappeared in hospital already. Bonus: The arthritic joints are no more. Bonus: The dry eyes are no more. Bonus: The eye floaters and spots have either gone or shrunk in size. Bonus; I have ear wax again. I am now off statins and diuretics, but I have no connection between that and the gelatin. Gelatin = collagen = connective tissue = joint grease. The diuretics leach your electrolytes. Script Slow-K comes with the meds, but does not really help.
Patrick Holford definitely has something on it when he says the elderly body does not have the same uptake abilities as the younger body. The overfeeding works. And the local supermarket now stocks decent supplies of gelatin. I told others and it seems a market was created for the stuff.
Sometimes I do experience cramps during the day. Then, At Night, before turning in I take about a pinky end of salt in coffee. No more waking up to agonizing cramps at three in the morning. Do be careful here. Balance it, because if you do not have enough salt inside, your muscles won’t fire! Did that one too. Oh yes, Only table salt, Sodium Chloride, works here.
Then the garlic.
In 2014 I contracted a skin disease. Itches like mad. I now understand how it can literally drive you insane. Cortisone, High SPF creams, Epizone E type washes, nothing helped. Beginning Feb this year I knew this thing is going to kill me.
Thank you Marjorie, from one thing and the other you led to me using five big cloves (big thumb size) per day on bread and cheese. Chew it like a chipmunk in the cheek to save the tongue. Tea to rinse it, but it works. Funny thing though, I had to leave off doing this for a few days on several occasions and my legs became waterlogged again with the itch starting up as well. The doctors say this is bad circulation, but the exclusive way in which this happens says something else to me. The garlic gets my legs back in shape again. No water. It usually takes about five days before the itch dies down completely again, after such a lapse. The cortisone still does help to get the bad local itches in trim. Mostly on the hands and feet.
The itch has largely gone, but I think there is a long haul ahead before this thing is truly dead.
Tea tree oil is marvellous for foot fungus. Just use your fingers to apply directly to your toes after shower. No waste.
Superbugs.
Two weeks ago I went to hospital with a cough. Could hardly breathe. After examinations, chest X-rays etc. I was told “there is a little infection”. Got an overnight Amoxicillin. Next morning the script went like this Amoxiclav 1000mg, 2×5 days. mg Azithrocillin 500mg, 1×3 days, Prednizone 50mg, 4 at once x 7 days. That is 1700mg per day. Some small infection. It is only today that I am well clear of it.
We need to seriously consider this situation and how we can protect ourselves against these. Actively do something like the Four Thieves Tonic. The allicin in garlic works. Period.
Something else.
I don’t know if you know of Maria Treben; Health through God’s Pharmacy (Germany) and Margaret Roberts (Regarded as the doyen of herbalism in South Africa, now passed away, her daughter is still active). Pharma Germania has a website and an online shop with slews of information per PDF.
I am not connected to these people in any way. It is just such a relief that I could find solutions that I want to share what I know. Please use it with care and keep an open mind. When you use different things, change one thing only over a period of time to connect the effect of it directly. Set up a regime for it, then change something else. I tell it as it stands so that you can make your own sense of it.
Thank you very much for these important tidbits of information. If you get sinus pressure or a runny nose, eat one-inch of fresh rosemary. Chew it up and swallow it, it actually reduces the runny/stuffy nose.